Swine, SRC and poultry lameness
Small ruminant orthopedics
As with cattle, lameness in small ruminants is a major cause of economic loss due to impacts on fertility, milk and fiber production, animal growth and animal well-being.
Common causes of lameness in small ruminants include contagious foot rot, hoof horn disorders, poor foot conformation, retrovirus-associated arthritis/synovitis (CAE and OPP viruses), bacterial polyarthritis caused by Mycoplasma and Chlamydia spp., and white muscle disease.
Goats tend to lift or minimize weight bearing on an affected limb. Bilateral issues will lead both sheep and goats to adopt different postures for eating and walking (eg eating on their knees). More subtle lameness is detected by head nods and changes in stride length.
Foot disorders
As with many LA species, most lameness issues are due to foot conditions.
The main foot issues are foot rot (biggest concern), contagious ovine digital dermatitis (growing concern), ovine interdigital dermatitis (foot scald), white line disease (shelly hoof), sole ulcers (called laminitis) and pedal joint infection. Dichelobacter nodosus, Fusobacterium necrophorum, Treponema spp., and Truperella pyogenes are the most significant foot pathogens. The organisms are similar to those affecting cattle.
As mentioned below, some sheep are resistant to contagious foot rot. Genetic susceptibility or resistance to white line disease has also been reported. Otherwise the risk factors are very similar to those reported in cattle. Overgrown, cracked or damaged hooves are more prone to secondary issues. Sheep with lower body condition scores and at higher production levels have more issues. Environmental and management conditions impact disease risk.
Foot disorders can be minimized by keeping animals in a dry environment and on a good nutritional plane. Good foot trimming is essential and proper foot baths or antiseptic sprays can help, particularly when animals are housed on soft footing. If an animal is lame, treatment should be instituted within 3 days for optimum results. Grouping animals at the time of hoof trimming, trims that damage the hoof wall and trims using contaminated equipment can all increase the spread of Dichelobacter. To minimize the spread, any equipment should be wiped down with alcohol, personnel should wear gloves and should change them for each animal. All horn trimmings should be disposed of.
Contagious digital dermatitis
Similar to digital dermatitis in cattle, Treponema (spirochete) infections cause digital dermatitis in both sheep (contagious ovine digital dermatitis; CODD) and goats (caprine digital dermatitis; CDD). However, unlike cattle in which lesions stay at the coronary band, things can get much worse in sheep. While the infection starts at the coronary band level with either proliferative or ulcerative lesions, the infection will extend into the hoof, undermine the hoof wall and eventually lead to avulsion of the hoof capsule. [This is in contrast to bovine digital dermatitis which stays above the coronary band and is not associated with hoof wall issues.] Due to damage to the coronary band, hoof regrowth is often abnormal.
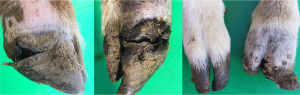
Topical tetracycline is recommended for CODD, as it is for bovine digital dermatitis. Severe infections may require digit amputation. Control is via maintaining closed herds, foot baths, disinfection of trimming equipment and potentially vaccination. It may be prudent to avoid co-grazing sheep with cattle that have digital dermatitis. Digital dermatitis seems to be a worsening problem in sheep. In 2017, over 50% of UK flocks were affected. Caprine digital dermatitis is a similar problem and can also be difficult to treat.
Foot scald and foot rot
Foot scald and foot rot typically arise due to interdigital trauma and/or macerated skin from wet conditions. When just the interdigital space is affected, this is often referred to as “foot scald” [although more akin to bovine foot rot]. The interdigital space will be red with slimy exudate and a foul odor due to Fusobacterium infection. The skin may become ulcerated and necrotic. Affected animals may graze on their knees.
In small ruminants, foot rot is a higher level of severity compared to foot scald. In sheep and goats, foot rot occurs when the interdigital dermatitis has been exacerbated by Dichelobacter nodosus infection. Dichelobacter produces an enzyme that can dissolve hoof horn. Dichelobacter enzymes can undermine the sole and/or loosen the hoof wall. This can cause hoof wall detachment and/or subsequent abnormal hoof growth. The level of enzyme activity varies by strain of Dichelobacter.
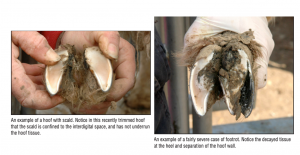
Treatment includes topical copper sulfate (drying agent) for foot scald and/or systemic antibiotics for foot rot affected animals, ensuring a clean and dry environment, weekly foot baths (impractical for most) and appropriate foot trimming regimens. Biotin supplementation may help speed recovery. During recovery, it is important to ensure animals are able to reach food and water; very lame animals will not be willing to move with the flock. Many will need NSAIDs. Animals that do not respond should be culled for humane reasons.
Prevention is key. Precursors to the disease include overgrown, cracked or damaged hooves; regular trimming is recommended. While foot scald is primarily due to environmental contaminants and environmental factors, it is important to keep Dichelobacter out of the sheep/goat herds. Dichelobacter does not persist very long in the environment – it only lasts a month or two. The main source of infection is feet of infected animals, where it can persist for years. Lame animals should not be brought into the flock. Any new or returning animals should have feet inspected and be quarantined for 30 days; however, it is easy to miss carrier animals! Foot trimming equipment should be cleaned properly.
Some sheep are genetically resistant to foot rot. Merino sheep are known to be prone to foot rot. Vaccines for Dichelobacter exist but have relatively short duration of action (<6 mo) and are not totally effective unless adjusted for circulating serotypes. Injection site reactions are high. Multivalent vaccines are not recommended but footbaths have been shown effective at controlling Dichelobacter. Unfortunately, footbaths have also been associated with transmission of infectious agents to other sheep. Topical oxytetracycline had comparable cure rates to footbaths. Antibiotics are effective; farmers may be reluctant to use them in lambs due to meat withholding requirements.

Other foot lesions
Interdigital fibromas do occur but are uncommon. Surgical removal is usually curative.
Toe granulomas typically occur due to over-trimming (toe region). These can be hard to treat. The granuloma can be shrinked with a mixture of sugar+iodine. Undermined horn needs to be removed. Prevention is by maintaining a good digital cushion and avoiding aggressive or unnecessary trimming.
Milking goats may develop metabolic issues that lead to laminar inflammation. Or not. We used to consider this a problem in cattle but now we think this is more related to changes in the suspensory ligaments.
Goats with foot pain due to metabolic issues may be found walking on their knees. Hoof growth may also be abnormal. Goats can also be affected by interdigital dermatitis, foot cracks and heel bulb erosions.
Foot and mouth disease will cause lameness due to lesions at the coronary band and in the interdigital tissues. Remember that ulcerative lesions require reporting to the Department of Health in the US.
Joint disorders
Septic arthritis is typically due to hematogenous spread in neonates (16% had an umbilical infection) and due to trauma in adults. Infections due to trauma are treated like they are in other species – joint lavage and antibiotics. In neonates, the entire animal needs treatment due to the septicemia and the inciting cause also needs to be treated (the umbilical infection, etc). Joint flushes are still needed, as well.
Chlamydial polyarthritis is a common contagious disease of feedlot lambs and likely occurs in goats, as well. Disease occurs in 1- to 8-month-old lambs, with 3- to 5-month-old lambs most commonly affected. In feedlots, outbreaks often occur a few weeks after lambs are introduced. Animals are febrile and reluctant to move. Multiple joints may be swollen. Chlamydial conjunctivitis can be seen simultaneously. Joint cytology may show elementary inclusion bodies. ELISA and PCR testing is confirmatory. Morbidity can be as high as 80% but mortality is very low; most cases resolve without treatment in 10-14 days. Antibiotic therapy (erythromycin, tylosin, tetracycline) will speed recovery.
Mycoplasmal arthritis is a highly fatal disease of goats. Affected animals show signs of polyarthritis, septicemia, and mastitis. In the United States, most outbreaks are in large goat dairies. Morbidity and mortality rates as high as 90% have been reported in kids. The organism is usually introduced to the farm by an asymptomatic shedder. Antibiotic treatment does not usually resolve the infection. Prevent the disorder by feeding only pasteurized milk to goat kids.
Erysipelothrix polyarthritis is typically seen in 2- to 6-month-old lambs but it can also cause neonatal joint infections. Outbreaks may affect as many as 40% of the lambs in a flock. Animals present with fever and lameness but minimal joint swelling. Erysipelothrix polyarthritis will progress to chronic arthritis if not treated appropriately.
Infection with caprine arthritis – encephalitis virus (CAEV )is widespread and chronic polyarthritis is the most common finding. Most infection is transmitted from doe to kid through the milk. Venereal disease and horizontal transmission are possible. Four clinical syndromes have been described for CAEV-infected goats: arthritis, leukoencephalomyelitis, interstitial pneumonia, and mastitis. Most animals are asymptomatic but are infected for life. Chronic progressive arthritis is seen in goats older than 6 months and is usually characterized by swelling of one or both carpal joints. Arthritis may affect other joints but it usually not detected. Signs may wax and wane initially. Some animals deteriorate over a few years while others remain stable for much longer. Combining ELISA and PCR with repeated testing is the best way to detect positive animals. No treatment is available. Ovine progressive pneumonia is a similar disease in sheep that only occasionally affects joints.
Lyme disease (Borrelia burgdorferi) does affect deer, sheep and occasionally goats. Testing is challenging. Sheep seem to be able to avoid systemic infection but can enable tick to tick transmission. A typical treatment regimen is a 2- to 4-week course of oxytetracycline, ceftiofur, or penicillin. Prevention of the disease currently relies on tick elimination.
Degenerative osteoarthritis is relatively common in older animals and can be exacerbated by CAEV. Elbow OA seems to be particularly prevalent. Elbow joints will not have much effusion but will have decreased range of motion. Animals may have a stiff gait and many have overgrown feet. Disease is usually advanced by the time of diagnosis. Treatment is focused on NSAIDs but can include joint protectants and surgical arthrodesis.
Physitis and osteochondrosis are found in rapidly growing animals.
Bone disorders
Osteomyelitis can occur due to trauma or hematogenous spread. Signs include lameness, pain on palpation, and focal swelling. Animals may be recumbent. Radiographic changes may not be visible for up to two weeks. Prognosis is guarded.
Rickets and osteomalacia can occur in young animals due to deficiencies in Vitamin D, phosphorus and/or calcium. Corriedale sheep can develop inherited rickets. Signs may include stiff gait, shifting legs, lameness, and recumbency due to bone fragility and pathological trauma. Joints and bones of the distal aspects of the limbs may be enlarged along with enlargements of the ribs at the costochondral junctions (rachitic rosary). Limbs may be bowed (angular limb deformities). Teeth may be mottled and their eruption delayed. Treatment is based on Vitamin D3 injections.
Fibrous osteodystrophy (nutritional hyperparathyroidism) may be seen in animals on a high phosphorus diet. Animals have a big head/rubbery jaw due to replacement of bone by fibrous tissue.
Fractures and other injuries can be treated fairly effectively due to the ruminant healing potential and small size. Amputations are a possible option, as are limb slings. Schroeder-Thomas splints can be effective at fracture stabilization when a cast is not appropriate.
Muscle disorders
- Blackleg– Clostridium myositis
- Sarcocystis– intracellular protozoan parasite; typically asymptomatic in animals but issues in people
- Nutritional muscular dystrophy– deficiency of selenium, Vitamin E or both; white muscle disease
Congenital disorders
- Spider lamb syndrome/ Hereditary chondrodysplasia
- Suffolk and Hampshire breeds are at greatest risk for this inherited condition
- Chondrodysplasia may be seen at birth or develop within the first 6 weeks of life
- Caused by a mutation in the fibroblast growth factor receptor 3; testing is now available
- UC Davis spider lamb information and testing
- A similar condition is found in beef cattle with hypomagnesemia
- Arthrogryposis
- congenital fixation (contracture) of multiple joints associated with a variety of teratogens
- inherited arthrogryposis has been reported in Suffolk and Corriedale sheep. Autosomal recessive mutation.
- also caused by Schmallenberg virus
- Polydactyly
- likely inherited
- Patellar luxation
- Affected animals will crouch due to inability to straighten the hindlimbs
- differential – femoral nerve injury due to dystocia (rare in small ruminants)
- genetic predisposition?
- may not ingest colostrum due to inability to stand and nurse
- surgical imbrication +/- trochleoplasty
- Myotonia congenita / Fainting goats
- tetanic contraction when startled
- autosomal dominant trait
- Spastic paresis
- constant contraction of gastrocnemius muscle -> leg extended behind and back arched
- considered inherited
- Flexural deformities
- treat as for foals with oxytetracycline and bandaging
- if surgery is needed, just cut the flexor tendons versus cutting the check ligaments
- most are congenital
Key Takeaways
Foot issues are still predominant. Sheep and goats get an infectious form of foot rot that can be devastating to flocks/herds. Infectious digital dermatitis can lead to hoof avulsion and is spreading through flocks. The same prevention and maintenance as for cattle helps minimize issues.
Some breeds have a genetic resistance to hoof disorders.
Goats also get several infectious forms of arthritis.
It is difficult to find good numbers for treatment response rates.
Fracture healing and repair typically carries a good prognosis. Limb and digit amputations are options.
Practice
Resources
Is footbathing as effective as antibiotics when treating sheep with footrot or contagious ovine digital dermatitis? VET RECORD | 23/30 September 2023- nice discussion of pros/cons
Ovine footrot: A review of current knowledge. The Veterinary Journal 271 (2021)- Nice review but the abstract tells most of it. Good pics
Pain management in small ruminants and camelids: Analgesic agents.Vet Clin North Am Food Anim Pract . 2021 Mar;37(1):1-16
Aetiology, Risk Factors, Diagnosis and Control of Foot-Related Lameness in Dairy Sheep. Animals (Basel). 2019 Aug; 9(8): 509.
Sheep, goat and cervid medicine. 3rd ed. Elsevier, 2021, Ch 11. Diseases of the musculoskeletal system.
Musculoskeletal Disease including Foot Disorders. In Goat Medicine and Surgery. 1st ed. 2017
Understanding contagious digital dermatitis. In Practice, 2018-03, Vol.40 (2), p.60-65
Ovine footrot: a review of current knowledge. The Veterinary J 271(2021)105647
-includes several videos with good pictures
Mindmap. downloadable file
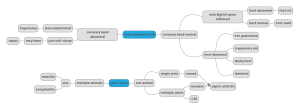
mass that forms when the immune system walls off a foreign substance.
inflammation of the growth plate or physis
defect in cartilage maturation process
the joint is bent (flexed) and cannot be straightened

