Equine podiatry
Subsolar (hoof) abscesses
Dr. F Tóth notes
Signalment
Hoof abscesses are common across all ages, sexes and breeds
Etiology
The cause is often unidentified but may be a penetrating wound (including horseshoe nail) or deep bruise. When a horseshoe nail hits the sensitive laminae, this can lead to trauma and infection. This is termed a “hot nail”. Horses with chronic laminitis are prone to hoof abscesses as the laminar interdigitation is damaged; this damage leaves an opening for bacteria. White line disease can also lead to abscesses due to similar structural damage.
Clinical signs
Horses develop a sudden, severe unilateral limb lameness. The horse is often reluctant to bear weight on the limb. The owner may believe the horse has a fracture.
On physical examination, the affected foot is warm and has bounding digital pulses. The distal limb (pastern area) is often swollen.
When the hoof is pared, a black spot may be visible in an area that is usually not black. For some reason, hoof pus is black.
The horse may develop a draining tract at the coronary band – “gravel” (I have no earthly idea why it is called a gravel). It is often easier for an infection in the foot to drain upwards rather than to break through the tough hoof wall or sole.
Diagnostics
Hoof tester examination
The horse will typically be very sensitive to hoof tester pressure. The entire hoof tends to be sensitive so localizing the abscess to a specific part of the foot is not always possible. In some cases, the hoof testers will squeeze out black goo from the abscess.
Hoof paring
Lightly paring the sole (removing the superficial layer) can help find the abscess. Look for a black spot that doesn’t pare off.
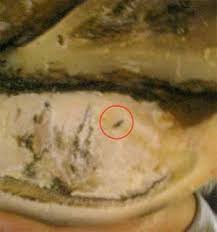
If no spot is identified, it can help to poultice the foot (eg Animalintex bandage) and/or to soak the foot in warm water mixed with Epsom salt. This softens the horn, making paring easier. The epsom salts may also help draw the abscess to the surface.
Nerve block
Pain from the abscess can be hard to totally numb but it should improve at least partially to a local nerve block (lateral or medial PDN or abaxial sesamoid block). Local anesthesia may be necessary to work on the foot due to the exquisite pain.
Radiographs
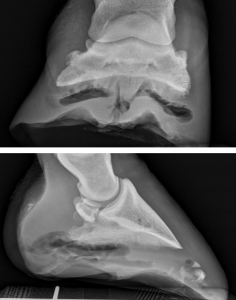
Radiographs can help rule out a fracture or laminitis. In some cases, the bacteria produce gas which can be seen radiographically. Radiographs can also identify bone involvement (chronic abscesses).
Treatment
The goal of treatment is to create ventral drainage for the infection. The procedure is usually done standing with or without local anesthesia. The tract should be opened just enough to establish drainage. We want to avoid further disrupting the hoof structure. Debridement should be stopped if blood or pink tissue is encountered.
After the abscess is opened, the foot is soaked in warm Epsom salts, treated with a penetrating hoof cleanser, or poulticed to encourage drainage.
The foot is bandaged to minimize contamination until the defect can be filled with granulation tissue or horny sole. If the defect is large, a shoe with a “hospital plate” may be indicated. This is usually a metal or rubber shoe covering that can be removed for treatment and then replaced to keep the foot clean.

Tetanus prophylaxis is indicated. Antibiotics are not usually needed. NSAIDs can be used as needed for pain. Once the abscess is open, the pain is usually substantially reduced.
Treating a Hoof Abscess 1 (Kaltura version w/ captions)
If the distal phalanx is involved (osteitis), then bone must be curetted. This requires general anesthesia and the application of a tourniquet. Curettage is most easily done through a trephine hole in the hoof wall. Regional limb perfusion with antibiotics is recommended.
Recent work out of UPenn suggests that carbon dioxide treatment might increase hoof growth. This could be useful when hoof wall has been removed and the foot is unstable
Prognosis
The prognosis is excellent for uncomplicated solar abscesses. However, the prognosis is guarded to poor if synovial structures or the pedal bone are involved (uncommon).
Key Takeaways
Hoof abscesses can be exquisitely painful (think after-effects of slamming your finger in a door).
- If the horse looks fracture lame but the limb seems okay, think hoof abscess
- It is easy for a shoe nail to cause trauma to sensitive laminae
- Abscesses need drainage – but try to limit damage to the sole or wall
Resources
Horse hoof abscesses, UMN extension
What is your diagnosis, JAVMA | DEC 1, 2021 | VOL 259 | NO. 11-keratoma
Other Clinical Problems of the Equine Foot Vet Clin Equine 37 (2021) 695–721

