Large animal wounds
Wound management
Medications
NSAIDs will slow wound healing but so will swelling. NSAIDs are useful to control the initial inflammation (first 72 hours) but then should be discontinued. Most horses are not painful after the incident. Signs of pain would indicate deeper trauma to bone, tendons or ligaments.
Horse NSAIDs – phenylbutazone, firocoxib, flunixin meglumine
Food animal NSAIDs- flunixin meglumine (approved), meloxicam (off label use)
Systemic antibiotics are generally not indicated unless deeper structures are involved or infection would be life threatening (eg near the chest or abdominal cavity). In these cases, iv antibiotics may be needed.
Regional perfusion of antibiotics can help with deeper wound management in the distal limb. For regional perfusion, a tourniquet is placed on the limb and a dose of antibiotics given iv below the tourniquet, concentrating the drug in the area needed. Antibiotics may also be injected directly into the synovial structures.
 Regional limb perfusion performed on a cria
Regional limb perfusion performed on a cria
Once granulation tissue has developed, it will protect the wound from outside contamination. This typically means antibiotic coverage is needed for about 5 days maximum or just until granulation tissue covers the wound.
Tetanus toxoid
Horses and small ruminants are very sensitive to Clostridium bacteria and to tetanus infection. Any wounded horse, goat, sheep or camelid should be boostered with tetanus toxoid if it has been more than 6 months since the annual vaccine. If a horse has a deep wound and no history of tetanus toxoid, the horse should also be treated with tetanus antitoxin. Tetanus antitoxin does carry the risk of serum sickness (immune response to equine antibodies) and is not given if the horse has been vaccinated previously.
Wounds left to heal by second intention generally do very well, particularly those above the hock or carpus. The wounds should be kept clean and dry, potentially covered by a water based ointment to maintain tissue moisture. Lower limbs may be bandaged until granulation tissue fills the defect. Wounds on the upper limbs or torsos may be difficult to bandage and bandaging is often not necessary.
Wound debridement
Sharp debridement (using a scalpel to remove damaged or contaminated layers) is less traumatic than rubbing and scraping the wound to remove debris. Tissues are debrided back to bleeding layers, minimizing debridement to critical structures and over joints.
NOTE: Eyelid wounds should not be debrided; this area has good blood supply but do not tolerate missing skin. Never trim the flap of an eyelid wound; all parts should be reconnected to avoid lid margin scarring and exposure keratitis. If concerned, these cases should be referred. See Eyelid lacerations
For some regions, sharp debridement might open closed structures (joints, tendon sheaths, body cavities). In those instances, wet to dry bandages or chemical debridement may be used. For wet to dry bandages, damp gauzes or other bandaging products are applied to the wound. At the next bandage change, those bandages have dried out; when removed, they remove any dead cells with them along with wound exudate. Medical maggots can also be considered for more wounds with deep contamination.
Wound closure
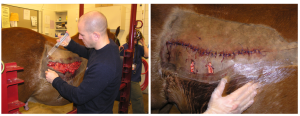
After complete evaluation and cleaning, the veterinarian must decide if the wound should be closed primarily, managed with delayed closure or left to heal by second intention. Many wounds cannot be closed, making the decision easy. If closure is possible, most vets will attempt it. However, it is important to avoid creating an abscess in the area. Ensure the wound can drain ventrally if needed. Often this is most readily done with an incision at the ventral aspect or by leaving the wound partially open. If the incision is made perpendicular to the lines of tension, it will stay open longer. Penrose drains can be used; these should not exit the wound or incision and should be pulled in 2-3 days as they create additional inflammation.
While delayed primary closure can be useful in small animals, in large animals it doesn’t often work as wound retraction occurs, enlarging the wound surface area and making it even harder to close.
Expect dehiscence in areas of high motion or high tension. Warn owners that the wound may fall apart in 2-3 days. Managing the swelling may help. Distal limb casts can support the wound and allow primary closure.
Topical wound agents
If the wound cannot be closed, topical salves may help keep tissues moist and minimize wound healing delays. Water soluble ointments are preferred over oil based ointments. Agents should be safe for new epithelial cells. Avoid toxic compounds. Generally triple antibiotics (neomycin + polymyxin + bacitracin) or silver sulfadiazine are used. Recent work suggests silver sulfadiazine should be avoided in acute wounds due to its cytotoxicity. Nitrofurazone (yellow goo) and chlorhexidine (blue goo) were used historically but are less commonly used now. Various bacteria can grow in nitrofurazone and it can actually delay wound healing. Chlorhexidine has been shown safe. Efficacy is unknown. Medical grade honey may even improve wound healing and decrease the risk of dehiscence if applied prior to closure.
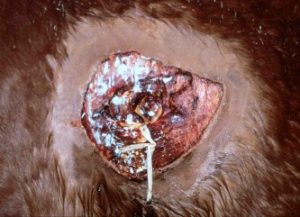
Many horse owners will want to apply various solutions to the wound to prevent proud flesh (exuberant granulation tissue) formation. While most of these agents do control proud flesh, they also damage the new epithelial cells. If needed, corticosteroid cream can be applied in a light layer once weekly.
Drains
Penrose drains can be used to assist drainage of wound fluids. They should not be exited out an incision or healing wound but should exit the most ventral aspect of the pocket. Remember: drains are foreign bodies and will cause additional inflammation. Drains can also wick bacteria into the wound. Generally a drain should be removed in 3-5 days or when the drainage slows. Do not expect drainage to stop with a drain in place. In many cases, extending the incision to the ventral aspect or creating an incision for ventral drainage is more effective.
Restrict motion
Limiting motion will improve healing. Stall rest without hand walking is recommended at least initially. Bandages and splints may be useful. Horses don’t often like stall rest and extra attention may be needed to improve horse and owner attitudes, including drugs and enrichment activities (for the horse).
Bandaging – lower limb wounds
Generally horse wounds are bandaged initially to prevent further contamination. Bandages do promote granulation tissue formation so are generally only needed in the initial stages of wound healing unless the limb is unstable or bandaging is needed to minimize motion.
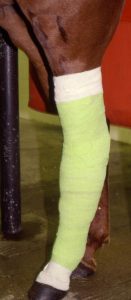
Antibiotics and/or antiseptics may be applied to the wound and then the wound covered by a nonstick pad that is held in place with a soft wrap. A support wrap is then placed on the limb. This is often a manufactured bandage or sheet cottons. This layer is held in place with brown gauze or vetwrap. The brown gauze and/or vetwrap is applied snuggly with even tension. Bulges or bumps in the support layer can lead to tendon damage. A bandage that is too loose will fall down, creating folds and bulges. If brown gauze is used, vetwrap is placed over it to provide a bit more pressure and keep everything in place. Finally, tape may be used to cover the openings at the top and bottom of the bandage to minimize contamination.
After granulation tissue fills the defect, bandaging of lower limb wounds is generally contraindicated. Exceptions include wounds near the ground or in very contaminated environments. Occasionally horses will chew at the wounds; these wounds may need bandaging for protection (and additional methods to prevent chewing may still be required).
Casts (either incorporating the foot or over a bandage) can be used instead of cotton padding. These stabilize the limb more effectively and can be cost neutral. Casts can be very useful if you have sutured the wound and/or in cases when regular bandage changes might be problematic
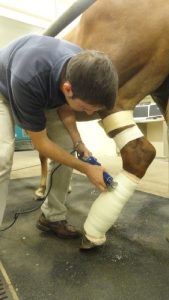
This horse is receiving an iv regional infusion of antibiotics (note the tourniquet just below the stifle) and has a bandage cast (cast placed over a layer of padding). The cast is being bi-valved (cut into longitudinal halves) in order to make a two part splint that can be changed.
Casts should not be left on the hindlimb of young horses (<5 years of age) for more than two weeks. Severe osteoporosis leading to sesamoid bone fracture can result.
Bandaging – upper limb wounds
Bandages can be sutured over the wound if needed (stent bandage). Circular loops of suture are placed adjacent to the wound and a fresh towel or pad held in place by “laces” threaded through the loops.
Key Takeaways
The main steps for wound management are
- cleaning
- sharp debridement
- closure or management for second intention healing
- restrict activity
NSAIDs are helpful for the first 3 days. Antibiotics are typically not needed or are only needed until granulation tissue develops. Corticosteroid cream may be used weekly to control granulation tissue.
Horses are not always good patients. Warn your clients that any repair can fall apart – generally in 2-3 days.
Most limb wounds will need to heal by second intention. This means lots of bandage changes and prolonged stall rest. Topical antibiotics help everyone feel better for the first 5 days.
Resources
BEVA primary care clinical guidelines: Wound management in the horse. Equine Vet J. 2021;53:18–29.
Simple techniques to decrease tension on sutured wounds of horses. Equine vet. Educ. (2022) 34 (2) 67-72
Topical Wound Medications, VCNA Vol.34(3), pp.485-498, 2018
Equine Practice on Wound Management Wound Cleansing and Hygiene, VCNA Vol.34(3), pp.473-484, 2018
Things You Should and Should Not Put on a Horse’s Wound, The Horse, 2016
Wound Care in Horses, VCNA Vol.28(1), pp.83-100, 2012
proud flesh; granulation tissue that doesn't stop when the wound is filled but continues to grow into a mound

