Equine joint disorders
Septic joints
Etiology
Joint sepsis can occur due to trauma (puncture wounds and iatrogenic), extension from nearby infection and hematogenous spread. Hematogenous spread is unusual in adults; in foals it is usually related to umbilical, GI or respiratory infections. A variety of organisms can be identified with wounds, including anaerobes. Iatrogenic infections are often due to Staphylococcus aureus; these are associated with joint blocks and therapeutic joint injections. Systemic infections in foals are often gram negative coliforms. Rhodococcus equi can seed joints in older foals.
Diagnosis
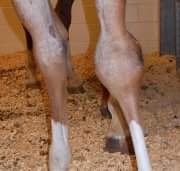
Early identification and aggressive treatment is required for soundness and often for life. Joint effusion and lameness are common. Foals may have a limited inflammatory response and lameness may not always be readily apparent. If you are suspicious of septicemia or joint infections, all joints should be carefully palpated and the umbilicus ultrasounded. Joint fluid should be sampled and submitted for culture and cytology. A healthy joint will have viscous fluid with low protein and low cell count. An infected joint will have high protein, a high cell count and low viscosity as inflammatory cells and mediators leak into the fluid and destroy the hyaluronan components and other proteins. The joint fluid and/or blood should be cultured to determine the causative agent and appropriate antimicrobial treatment.
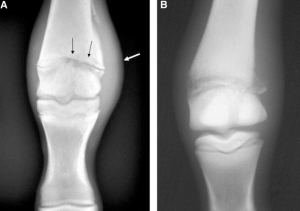
Radiographs are recommended as many cases of juvenile septic arthritis occur due to extension from an infected physis or metaphysis.
New
Recent research suggests that measuring enzymes (lysozyme and myeloperoxidase) in synovial fluid may be more effective at identifying septic joints and could result in a point of care test that could be used stall side. Watch for more work in this area!
Detection of synovial sepsis in horses using enzymes as biomarkers. Equine Vet J. 2022;54:513–522.
Treatment
Any underlying infection should be treated and infected umbilical stalks removed surgically if indicated. Systemic iv antibiotics are indicated; early administration may improve outcomes.
The joint is treated via lavage. Through and through needle lavage (two needles are put into the joint and fluid flushed into and out of the joint) is effective in foals and in very early cases of traumatic infection. If available, arthroscopic lavage is considered more effective in adults and in more chronic infections.
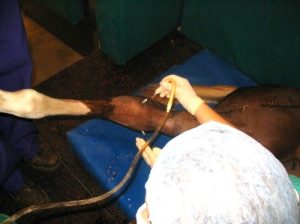
Local (intra-articular) antibiotic infusion of amikacin or other high powered antibiotic is usually combined with systemic administration of more broad spectrum and first line antibiotics such as penicillin/gentamicin or a cephalopsorin until culture results are available. (Amikacin is often used systemically in foals). Antibiotics alone are not effective.
Synovial resection may be required to remove deep seated bacteria and damaged synovium.
Management
Joint samples are taken every other day to determine if repeated flushing or injection is required and to ensure improvement.
If the infection cannot be controlled, the horse should be euthanized for humane reasons.
Prognosis
Prognosis is guarded. In general, if multiple synovial structures are involved or if other tissues are infected (bones, tendons, etc) the prognosis is decreased. Horses that received systemic antimicrobial treatment prior to referral had a better prognosis. Early identification and treatment is likely beneficial but no “golden” period has been identified. This may mean that there is no safe zone when contamination occurs but infection has not set in; it may also mean prognosis is not significantly altered if it has been 12 hours vs 6 hours since wounding. Foals treated successfully for a single septic joint have a good prognosis for both survival and race careers, compared to their siblings.
Key Takeaways
Foals can develop septic arthritis due to hematogenous spread. Adults develop septic arthritis due to wounds and injections.
Septic arthritis can result in euthanasia
Treat with lavage and antibiotics (local +/- systemic)
Resources
Current treatment and prevention of orthopaedic infections in the horse. Equine Vet Educ. 2023;35:437–448. Excellent review. Download if planning on an internship or residency.
Haematogenous septic arthritis, physitis and osteomyelitis in foals: A tutorial review. Part 1. Equine vet. Educ. (2021) 33 (12) 659-672
Haematogenous septic arthritis, physitis and osteomyelitis in foals: A tutorial review. Part II. Equine vet. Educ. (2022) 34 (1) 37-48
Septic Arthritis, Physitis, and Osteomyelitis in Foals, VCNA August 2017, Vol.33(2), pp.299-314
Antimicrobial selection for the equine practitioner, VCNA 2021, Vol 37, pp 461-494. Includes specific recommendations for musculoskeletal infections
Effect of arthroscopic lavage and repeated intra-articular administrations of antibiotic in adult horses and foals with septic arthritis. Veterinary Surgery. 2017;46:1008–1016.

