47 Weight loss
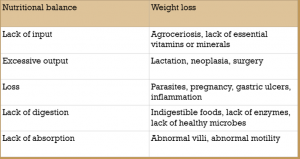
Weight loss occurs for five main reasons:
- Insufficient calories
- Lack of intake
- Excessive utilization
- Loss of protein or nutrients
- Skin
- Kidneys
- GI Tract
- Maldigestion
- Malabsorption
- Liver disease
Weight loss is often associated with hypoalbuminemia and potentially hypoproteinemia.
Insufficient calories
Insufficient calories can be due to insufficient intake (agroceriosis) or less intake than calorie usage. Increased calories are required with exercise, pregnancy, lactation, hyperthyroidism, parasitism, neoplasia and chronic illnesses.
Protein loss
Loss of proteins can occur through the skin (typically with burn injuries), the kidneys (proteinuria), and the gut. Gut loss maybe associated with ulcers and erosions, inflammatory bowel disease, tumors, crypt cell proliferation, increased lymphatic pressure, and tight junction disruption.
Maldigestion
Maldigestion is associated with liver or pancreatic issues in monogastrics. If the liver doesn’t produce or recirculate adequate bile, fat digestion is impaired. If the pancreas doesn’t produce functional enzymes, digestion of most dietary substances is impaired. In herbivores, if the microbes are not functional, cellulose digestion is impaired.
Malabsorption
Malabsorption is related to abnormalities in the intestinal wall. This may be due to diffusion or transport issues. the villi must be normal for good absorption. Malabsorption will occur if villi are lost, shortened or thickened. if diffusion gradients are not maintained, absorption will also be impaired. Glucose and protein digestion require active transport and short diffusion distances. Fat absorption is primarily diffusion.
Evaluation
Nutrient analysis can help identify if caloric intake is adequate. If the diet appears sufficient, laboratory testing should include a complete blood count, serum profile, urinalysis and total throxine (T4, cats). Additional testing may include fecal examinations, thoracic or abdominal radiographs, rectal biopsies, and abdominal ultrasounds.
Malabsorption (lack of protein absorption) can be difficult to distinguish from protein loss, particularly protein-losing enteropathies. Often both loss and malabsorption coexist. Low protein can also develop with renal disease, burn wounds, and liver disease.
Alpha-1 proteinase inhibitor to rule-out protein loss
Protein loss can be identified in dogs and cats by measuring alpha-1-proteinase inhibitor. This protein leaks into the intestinal lumen with severe disease but isn’t digested so can be measured in the feces.
Malabsorption tests
Intestinal malabsorption can be measured through 1) D-xylose absorption tests (proximal small intestine) or 2) Vitamin B12 (cobalamin) levels (distal small intestine). Low folate levels may also indicate proximal small intestinal disorders, particularly in cats. In large animals, ultrasound is often combined with duodenal or rectal biopsies and/or abdominocentesis. Additional tests tend to be specific for differentials, such as fecal parasite checks, Lawsonia titers, etc.
D-xylose absorption
D-xylose is a plant sugar that isn’t normally found in the bloodstream and is readily absorbed. D-xylose is administered orally and then blood levels measured. If blood levels do not rise sufficiently, malabsorption is diagnosed. If weight loss is present and D-xylose levels are normal, the problem is more likely to be maldigestion (e.g. pancreatic dysfunction). A flattened peak suggests malabsorption while a delayed peak correlates with delayed gastric emptying.
Cobalamin levels
Cobalamin is an essential co-factor in many mammalian enzyme systems. It comes exclusively from bacteria and is important in amino acid metabolism and DNA synthesis. Absorption is highly complex.
Dietary cobalamin is tightly bound to animal-derived dietary proteins. These proteins are partially digested in the stomach and the cobalamin released. It immediately binds to haptocorrin (aka R-protein). In the small intestine, the haptocorrin is digested and the cobalamin freed again. This time it immediately binds intrinsic factor. Intrinsic factor/cobalamin complexes are absorbed in the ileum. As it is absorbed into the epithelial, the intrinsic factor is removed and cobalamin released into the circulation. In the circulation, cobalamin binds transcobalamin II and is stored in the liver and kidney. (This is different than in people where intrinsic factor is released in the stomach).
Cobalamin deficiency in dogs and cats is generally associated with severe intestinal disease and with exocrine pancreatic insufficiency. Almost all cats and most dogs pancreatic insufficiency are cobalamin deficient, likely related to lack of intrinsic factor. Small intestinal disease must be chronic and severe to see cobalamin deficiencies as body stores are large. Hereditary cobalamin deficiency can also occur in some dog breeds.
Maldigestion tests
Maldigestion can be assessed through 1) trypsin-like immunoreactivity, 2) folate levels and 3) cobalamin levels. Additionally, enzyme levels can be measured for gastrin and pancreatic lipase.
Trypsin-like immunoreactivity
TLI is a more accurate measure of pancreatic function than lipase or amylase levels. Species-specific TLI is considered the optimum test for exocrine pancreatic insufficiency (EPI).
Folate levels
Folate can only be absorbed in the proximal small intestine. Many bacteria produce folate but generally only in the large intestine which has no receptors for folate absorption. In cases of pancreatic insufficiency, bacteria can overgrow in the small intestine due to lack of pancreatic enzymes. This can lead to high levels of folate in dogs with EPI. Cats tend to have low folate levels with EPI as they also get intestinal damage that impacts the folate receptors.
Cobalamin levels
Cobalamin insufficiency is more likely to be associated with exocrine pancreatic insufficiency than with malabsorption as described above. However, if TLI is normal, cobalamin and folate abnormalities are more likely to be associated with intestinal malabsorption. (When you have bacterial overgrowth, they bind the cobalamin receptor and prevent cobalamin uptake into the cell so this also lowers levels.)
Key Takeaways
Resources
Treatment of obesity in dogs and cats, Today’s Veterinary Practice
Hyperthyroidism in cats, Washington State University

