Enteric System: Post-Weaning Pigs
Salmonella Typhimurium
Clinical importance
Salmonella is a well-known genus of bacteria, mostly because it is a zoonosis causing food poisoning outbreaks, widely reported by the media. Among the 2,400 Salmonella serotypes, three infect pigs: Salmonella choleraesuis, Salmonella typhimurium and Salmonella derby and among those only Salmonella typhimurium commonly causes clinical signs in humans. This chapter will focus on Salmonella typhimurium, which typically affects finishing pigs and is the most common serotype in North America.
Etiology and transmission
Salmonella typhimurium is a gram negative bacteria that colonizes the intestinal tract of the pig, and more particularly the ileum, caecum and spiral colon, through their Peyer patches.
The main route of transmission is feco-oral since the pigs start shedding the bacteria within minutes from infection and can continue to shed up to 5 months after recovery from the illness. Salmonella also infects the tonsil of the animal and can be shed in oral fluids leading to nose-to-nose transmission. More rarely, piglets can get infected by the sow. Salmonella is quite resistant in the environment and can be carried in the intestinal tract of birds and rodents, leading to indirect transmission of the pathogen. Identifying the source of the introduction in a herd is a challenge. Feed ingredients of animal origin, contaminated environment, and introduction of a positive animal are all plausible causes.
Non-clinical Salmonella infection is common across the US industry. In 2006, the National Animal Health Monitoring Service determined that 52.6 % of herds had Salmonella in their population (NAHMS). Clinical signs are pretty rare in commercial herds but can be found in clean, naive herds that have just been set up, or in stressed and immunocompromised ones.
Associated symptoms
The main symptom of salmonellosis is a yellowish diarrhea affecting pigs from mid-nursery all the way to market. Dehydration and anorexia are commonly seen among affected pigs. The initial episode does not last much longer than a week, but re-infection is common within the next 3 to 4 weeks. Mortality is rare and the majority of the pigs will completely recover. However, some individuals can remain carriers and sources of infection for up to 5 months after recovery. Some cases of rectal strictures have been reported after a clinical salmonellosis. In this case, pigs cannot defecate and intestinal contents remain trapped in the abdomen, creating a severe distension.
Associated lesions
Macroscopic lesions
Inflammation of the ileum, the caecum and the spiral colon is the most common macroscopic lesion. The most indicative lesion due to salmonellosis by Salmonella typhimurium is the presence of pseudomembranes in the intestine, described as yellowish, fibrinonecrotic debris giving the impression that the mucosa separated from the intestinal wall. Mesenteric lymph nodes are enlarged and inflamed. In more chronic cases, button ulcers can be easily spotted in the spiral colon.
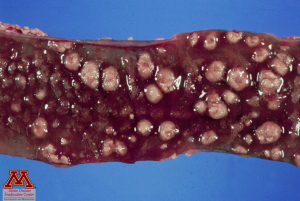
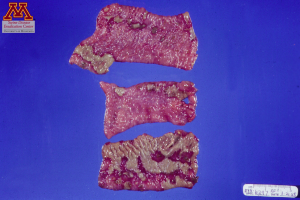
Button ulcers (left) and pseudomembranes (right) in the intestinal tract. Source: Dr. Carlos Pijoan
Microscopic lesions
Microscopic lesions are also usually seen in the ileum,caescum and spiral colon, often presenting as blood clots in nearby capillaries and damage in epithelial cells with presence of neutrophils and macrophages. Lymph nodes will also have a high number of neutrophils and necrosis may occur.
What is the most characteristic lesion associated with salmonellosis?
- Pseudomembranes in the small intestine
- Thickening of the ileum
- Mucus and fresh blood in the spiral colon
Diagnosis
Definitive diagnosis by clinical symptoms alone is difficult as many pathogens can cause diarrhea in pigs. Lesions found during the necropsy, such as pseudomembranes in the ileum or button ulcers in the spiral colon should be indicative of salmonellosis. Isolation of the bacteria along with clinical signs and lesions is the only way to get a definitive diagnosis. Salmonella can easily be cultured from colon samples. ELISA tests are becoming more popular and work well to determine the level of infection in the herd.
Differential Diagnosis:
There are a number of diseases that result in diarrhea of weaned pigs. Rotavirus, coronavirus, E.coli, ileitis and swine dysentery must be considered.
A positive culture from Salmonella typhimurium in the colon is sufficient to establish a diagnosis of salmonellosis. True or False?
- True
- False
Treatment, Prevention and Control
Antimicrobial treatments can be effective in decreasing the severity of the clinical signs and stopping the propagation of the disease among the herd but they are not appropriate for long-term management of the disease. Typically drugs such as apramycin, ceftiofur, trimethoprim-sulfonamide, or gentamicin can be used. Reports of antimicrobial resistance are common; it is recommended to test the isolated strain for susceptibility prior to implementing a treatment.
Preventing infection by Salmonella is very difficult, if not impossible since most of the US herds are infected. However, it can be controlled to the point where most pigs are subclinical and do not display clinical signs. Providing a clean, dry, and properly ventilated living space can lower stress and reduce the risk of developing the disease. Herd monitoring is difficult due to the prevalence of infection and the intermittent shedding of chronically infected pigs.
What makes Salmonella typhimurium a nearly-impossible disease to eradicate?
- There is no effective antibiotic treatment to limit the clinical presentation of the disease.
- Salmonella are difficult to culture, making the identification of positive animals challenging.
- Most of the US herds are positive for Salmonella typhimurium.
References
National Animal Health Monitoring Survey (NAHMS). 2006 https://www.aphis.usda.gov/animal_health/nahms/swine/downloads/swine2006/Swine2006_dr_PartIV.pdf

